
The Big Anti-Bullying Assembly

Posted on September 12, 2020 by Aliya Eastham - Uncategorised

This campaign is run by charity The Diana Award, a legacy to Princess Diana’s belief that young people have power to change the world. Join us on Monday 28th September for The Big Anti-Bullying Assembly 2020!
Posted on July 26, 2020 by Aliya Eastham - Uncategorised
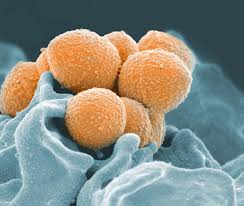
(https://gbss.org.uk/latest-news/group-b-strep-a-global-issue/)
Group B Strep (GBS or Strep B) is a bacteria carried by around 1 in 4 people.
Strep B causes sepsis, pneumonia and meningitis in babies.
Most Strep B infections in babies are early-onset, occurring in the baby’s first 6 days.
Late-onset Strep B infections are less common, and very rare after age 3 months.
Most early-onset Strep B infections can be prevented by giving antibiotics in labour to women carrying Strep B.
Strep B also causes infections in adults: in the elderly, women who are pregnant or around the time of childbirth, and in the immunocompromised.
Intravenous (IV) antibiotics given in labour are very effective at preventing early-onset Strep B infection. Worldwide, two strategies are used to select who to offer IV antibiotics to:
Most high-income countries routinely offer pregnant women a test for Strep B carriage and offer the IV antibiotics in labour to those whose result is positive, plus to those where other risk factors are present. Middle and low-income countries usually either use risk factors to determine who to offer the IV antibiotics in labour, or have no policy.
Countries that offer routine testing have seen their rates fall. Using risk factors has not shown the same success.
For example, in the UK & Republic of Ireland, the rate of early-onset Strep B infection went up by 19% between 2000 and 2015, despite the risk-factor approach being introduced in 2003.
In the USA where screening is routine, the rate of early-onset Strep B infection fell by 86% between the early 1990s and 2018.
We urgently need a vaccine to prevent Strep B infections. A vaccine could:
Working to stop GBS infection in babies
Posted on May 25, 2020 by Aliya Eastham - Uncategorised
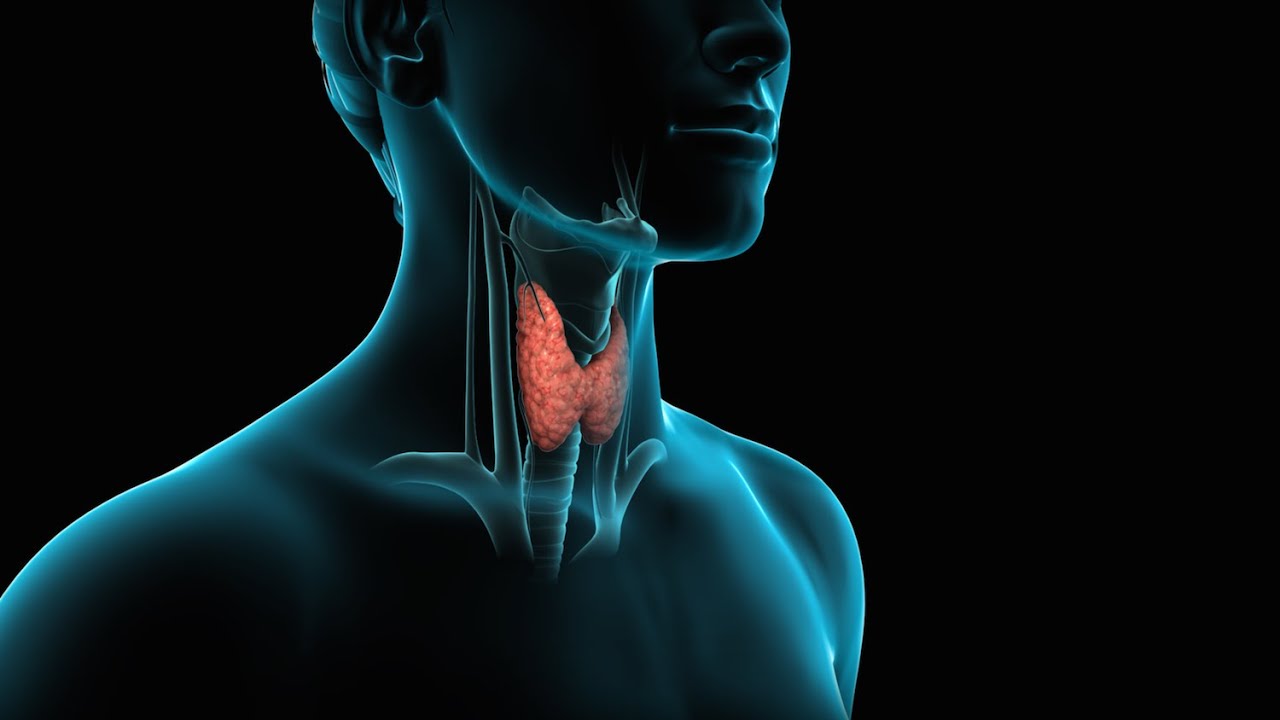
https://www.theinvisiblehypothyroidism.com/world-thyroid-day-25th-may-2020/
Every year, the 25th May is World Thyroid Day; an international event for raising awareness of what the thyroid gland is, what different thyroid conditions there are and symptoms of them, the importance of diagnosis and treatment, but also the many things that we face as thyroid patients.

The World Health Organization estimates that 750 million people worldwide have some form of thyroid disease, including 1 in 20 people in the UK say the BTF, but as many as 60% are undiagnosed.
Also, around 8 times more women are affected by thyroid disease than men, with key triggers being puberty, pregnancy and the menopause.
With these numbers, we have to keep encouraging anyone with symptoms of a thyroid condition to get it checked out via a full thyroid panel (also called a ‘thyroid function test). This includes TSH, Free T3, Free T4, thyroid peroxidase antibodies and thyroglobulin antibodies.
Monitor My Health is a new NHS Service. They offer a “Thyroid” finger prick home test which checks TSH, Free T3 and Free T4 for £29. They are run by the NHS, use NHS staff and labs and stand apart from other services for this reason. All profits also go back into the NHS. To check out their “Thyroid” home test kit click here.
World Thyroid Day could be the perfect reason to check these important thyroid levels.

The thyroid gland, located in the neck, is responsible for producing hormones needed for many bodily functions and processes. The main one is metabolic function. When thyroid hormone levels aren’t right, symptoms such as weight fluctuations, sensitivities to heat and cold, fatigue, hair loss, mental health conditions (such as depression and anxiety), dry skin and brittle nails can occur.
Symptoms for hypothyroidism can include: longterm fatigue, muscle aches and pains, sensitivity to cold, depression, weight gain, sleep disturbances, low libido, dry skin, hair and nails and feeling overall quite unwell.
Symptoms for hyperthyroidism can include anxiety, heart palpitations, unexplained weight loss, hot flushes, irritability and sensitivity to heat.
Symptoms of thyroid cancer may include neck pain, a hoarse voice, nodules/lumps and enlarged lymph nodes.
Symptoms of autoimmune thyroid disease (such as Hashimoto’s or Graves’) can include those mentioned above, including swinging test results and symptoms e.g. going through periods of better and worse health.
Although the thyroid gland is responsible for delivering crucial hormones that are needed for every function and cell of the body, a large percentage of the world’s population don’t tend to understand just how important this little gland is and what signs and symptoms to be looking for. As well as what tests they may need to ask their doctor about. This is why an awareness event can be so useful!
When a thyroid condition goes undiagnosed and untreated, many symptoms can persist and mount up. I had over twenty separate symptoms before my hypothyroidism and Hashimoto’s were diagnosed and treated.
There are many people living with the effects of an undiagnosed thyroid condition who could be healthier and happier once treated. When left untreated, symptoms can impact relationships, work lives, quality of life and more.
For those of us already diagnosed with a thyroid condition, we can gain awareness this World Thyroid Day about how to check our necks regularly for any abnormalities, what we can do to live well and which tests to have done.
We can also be aware of what results to look for, as many thyroid patients are still having ongoing symptoms.
I also encourage all thyroid patients to be their own health advocate and be an active participant in their own health and wellbeing. This includes understanding their thyroid condition.
As well as educating those around us on this butterfly-shaped gland, we should also take the time to educate ourselves! After all, knowledge is power and learning to advocate for ourselves gives us the best chance of recovering our health back to a good standard. See a list of thyroid websites here and some books here.

My book “Be Your Own Thyroid Advocate” also compiles all the information you need to begin advocating for your own health, in one place and in an easy to digest format.
World Thyroid Day is all about creating awareness of thyroid disease and disorders as a whole – for those going undiagnosed, those needing a review of their treatment and for those who feel good on their thyroid treatment, but can always learn some more and help spread awareness so that those who aren’t yet diagnosed, can be.
Posted on October 4, 2019 by Aliya Eastham - Uncategorised
When a woman suffers the loss of her baby, the grieving is inevitable. So, should we expect our partners to grieve with us, or be the pillars of strength through an emotional time?
This article first appeared in the February/March 2016 issue of Your Pregnancy magazine.
I was sat in Starbucks in Muscat, Oman, basking in that terrifying glow of fatherhood-to-be, when I got the phone call. Liz, who was nine-weeks pregnant in Cape Town, had had a miscarriage. I know my face turned white as a sheet. I know I almost threw up my coffee.

I know all the patrons were staring aghast at me as I stammered through the call. Within 24 hours, I was back in Cape Town to help my wife grieve.
Research from the British Miscarriage Association suggests that more than 50% of all pregnancies end in a miscarriage or stillbirth, but that almost half of all men whose partners miscarry never speak about their grief with their partner for fear of saying the wrong thing.
This, despite it affecting their own work and sleep. Men, it seems, are expected to return to normal life, with at best clumsy comments like, “Never mind, you can try again,” to tide them through their grief.
Certainly, to this day, not a single person has asked me how I was handling any of my wife’s three miscarriages. Not my male friends, not my mother, not my in-laws, definitely none of my wife’s girlfriends, and certainly not a grief counsellor.
No. This is what it means to be a man. Or so I thought. You are the rock against which the waves of her emotion break. Besides, you can’t have a situation where every adult in the house is a teary wreck. My tears seemed like a terribly selfish indulgence, especially when I saw my wife questioning her own value as a woman – a woman whose own womb had betrayed her.
And if the loss of a life within herself wasn’t devastating enough, her mistrust in her own body to do what it is designed to do, soured into a form of guilt which verged on self-hatred.
And suddenly, it seemed, the world was conspiring to inundate us with images of pregnant women – on TV, in movies, in books, on Facebook. Even the emaciated, homeless women sleeping in freezing rain in shop doorways seemed able to carry to term.
As a man, you want to fix things. And, if you can’t fix things, you want to move on. Am I right? Yes and no, according to South African mom Nicole Masureik, who started the support group Born Sleeping, in 2007, after having had a stillbirth. Nicole says men and women process grief very differently, especially when it comes to miscarriages.
The pregnant woman has a much deeper, constant, intimate connection with the life growing inside her, whereas for the man, this is still only a concept, a potential child, she explains.
“Whenever the miscarriage happens, or even if it is a stillbirth, many men feel they must be the stable rock, the provider who keeps the family going. This is a very typical male response, but unfortunately for women it’s the inappropriate response. She wants him to cry. She wants him to feel as devastated as she does. Of course he’s grieving, but this isn’t how men process their grief.
“Women are much more open with their grief. They talk to friends. They lie on the bed and cry. Men tend to be more internal. They keep themselves busy with work or physical activity. They might tell a close mate that they’re feeling down, and the mate will say, ‘Hmmm’, and they’re relieved that’s off their chest.”
Nicole’s partner Graeme Broster points out that after the stillbirth, “Nicole went into meltdown. My grief was less immediate. We had a one-and-a-half-year-old child, and somebody had to cook the meals, and do the school run. My grief had to be put on hold. The difficulty was coming back to that space so I could grieve. It took me about four years before I realised I hadn’t dealt with it, and it was still affecting my life.”
Nicole says that while women shouldn’t expect men to grieve in the same way as they do, men should not put expectations on the woman to sweep emotions under the carpet and to move on.
“In the last 10 years I’ve seen changes in society. When we first started this support group, men just didn’t ask for help for anything, certainly not for emotions. More and more, though, men are keen to come and talk things through in our counselling sessions. The next generation of young men are way more in touch with their emotions,” she says.
Joburg clinical psychologist Hlengiwe Zwane says often how men react to a miscarriage depends on several factors, including culture and individual personality, as well as whether the pregnancy was the result of months of planning and struggling to fall pregnant, or an unplanned pregnancy.
“If the couple are saying, ‘We’re pregnant’, you usually find a more collective sense of grief and responsibility for dealing with the loss. I’ve had women come to me who feel their partner doesn’t care. Then, when you meet the man, you realise he does care. He’s acting strong, but hurting on the inside.”
Zwane says the most important thing is to be real with one’s loss, to confront one’s grief and keep the lines of communication open within a relationship. “Speak to your partner. Is she feeling blamed, or carrying the guilt or blaming you? She needs you as much as you need her. Don’t delay or suppress dealing with your loss, as it will lead to unhealthy coping mechanisms, such as alcohol or drugs.”
Contact Born Sleeping at bornsleeping@gmail.com, or on Facebook: Bornsleepingza
Contact Hlengiwe Zwane on hlengiwe@jddp.co.za or 011 880 0921.
Posted on August 20, 2019 by Aliya Eastham - Uncategorised
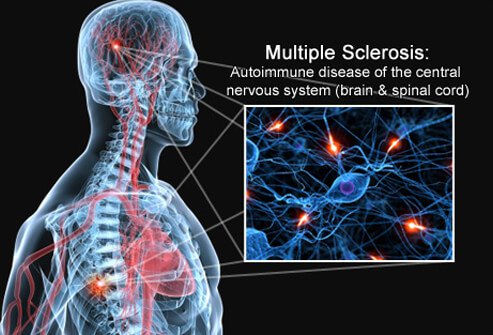
Around 100,000 people in the UK have multiple sclerosis (MS) (MS Society 2012), an autoimmune disorder of the central nervous system (Compston 2006). Most patients with MS present with a relapsing-remitting disease that, over years, typically leads to a progressive phase of permanent and increasing disability (secondary progressive disease) (Hawkins 2000). (https://www.acupuncture.org.uk/a-to-z-of-conditions/a-to-z-of-conditions/2817-multiple-sclerosis.html)
About 10–15% of patients have progressive symptoms from the outset, with no relapses and remissions (primary progressive disease). Some patients have a relatively benign form of the disease with no significant disability for many years (Hawkins 2000). The underlying pathogenic mechanisms in MS appear to be heterogeneous and involve inflammation and axon degeneration (Compston 2002).
Physical symptoms of MS commonly include vision problems, balance problems and dizziness, fatigue, bladder problems and stiffness and/or spasms (MS Society 2012). It can also affect bowel function, speech and swallowing, and cognitive function. Conventional treatment includes disease-modifying drugs such as interferon beta (-1b and -1a), fingolimod, glatiramer, and natalizumab, physiotherapy and dietary modification.
Compston A et al (Eds). McAlpine’s multiple sclerosis. Fourth edition. Philadelphia: Elsevier Inc, 2006.
Compston A et al. Multiple sclerosis. Lancet 2002; 359: 1221-31.
Hawkins C. Pathogenesis and clinical subtypes of multiple sclerosis. In: Hawkins CP, Wolinsky JS (Eds). Principles of treatments in multiple sclerosis. Oxford: Butterworth Heinemann, 2000.
MS Society. Signs and symptoms [online]. Available: http://www.mssociety.org.uk/what-is-ms/signs-and-symptoms?gclid=CPi8nuTBzLICFYYNfAodMnEAjQ
This Factsheet focuses on the evidence for acupuncture in MS.
There has been very little research published. One systematic review, which summarised and evaluated the available evidence of acupuncture for neurological diseases concluded that more rigorous trials are warranted to establish acupuncture’s role in MS. (Lee 2007) A randomised controlled trial that compared the effects of 2 types of acupuncture in 14 patients with secondary progressive MS found that minimal acupuncture resulted in greater improvement than Chinese medical acupuncture for psychological health: all other aspects were similar (Donnellan 2008). An uncontrolled open study, which looked at whether electroacupuncture diminishes voiding symptoms and improves quality of life in patients with MS and overactive bladder and urge incontinence, found that it may have a useful role in patients with MS and mild bladder dysfunction who do not wish to take medication or are unable to because of side effects (Tjon Eng Soe 2009). Both of these studies were tiny, so the results can be seen only as very preliminary.
In general, acupuncture is believed to stimulate the nervous system and cause the release of neurochemical messenger molecules. The resulting biochemical changes influence the body’s homeostatic mechanisms, thus promoting physical and emotional well-being.
Research has shown that acupuncture treatment may specifically help to relieve symptoms of multiple sclerosis by:
Posted on May 3, 2019 by Aliya Eastham - Uncategorised
A devastated mum has issued an urgent warning after her healthy three-month old baby died just hours after she took this happy picture of her (https://www.msn.com/en-gb/news/uknews/mums-warning-after-healthy-baby-dies-just-hours-after-smiling-in-happy-photo/ar-AAAQx8e?li=BBoPWjQ&ocid=mailsignout)
Fleur Edwards was completely fine and happy when she went to sleep in her cot alongside her parents.
But the 13-week old tot never woke up.
The day before Fleur died the family had attended a fundraising event for a relative.
Mum Emily Vandenbrouck, from Paignton, Devon, said: “Fleur had been held and kissed by lots of people that day – probably somebody held her who hadn’t washed their hands after using the toilet.
“I just want to raise awareness so that other families don’t have to go through the heartache that we go through every single day.”

© Provided by Trinity Mirror Shared Services Limited Mum Emily Vandenbrouck says Fleur had been held and kissed by lots of people the day before she died
Fleur had been featured in a happy family photo and been feeding normally and laughing just hours earlier.
But her condition deteriorated over the course of the night and it was later revealed that she had developed a fatal Group B Strep infection.
Now her grieving family and friends are holding a ‘Fleur’s First Birthday’ event to raise awareness of the condition that killed her.
Emily said: “She went to sleep completely happy and normal. No temperature. There was not a single thing wrong. She never woke up.
“She loved her sleep and slept through the night. She was the model baby. She was in our room. It was her dad who found her first. I grabbed her and did CPR but I knew as soon as I looked at her she was gone.
“We thought we were dreaming. For a couple of weeks I kept trying to wake myself up.
“That photograph was taken at 6pm the night before – it is very precious because it’s the only one of us all together.”

© Edwards family / SWNS A post mortem at Great Ormond Street Hospital for children found Fleur had died of a Group B Strep infection
Now family and friends including dad Ashley Edwards, sister Layloa, eight, and Rhys, five, have rallied around to help mark Fleur’s first birthday with a fete at Foxhole Community Centre on May 12 between 11am and 3pm.
Emily said: “This is my way of marking her birthday – it’s difficult to know what to do when your baby has died.”
The fundraiser will have four bouncy castles, golf, mascots, a DJ, children’s entertainer, face painting, hair braiding, glitter tattoos, forest school and a giant raffle with hundreds of pounds worth of prizes.
Doctors were surprised by Fleur’s death because even a spinal tap showed no sign of infection.
Eventually a post mortem at Great Ormond Street Hospital for children found Group B Strep.
Now Emily is trying to warn as many parents as she can about the infection and is angry about the lack of knowledge for mums.
She added: “I think it’s disgusting. Pretty much 90 per cent of people don’t know about this. I cannot believe how hushed up it is. I am a mother of three and I had never heard of it.”
“Fleur was the most content, smiley, model baby. She loved her sleep and she was very greedy – I was breastfeeding her and she got chubby very quickly.
“My mum said when she was born there was a magic about her.”
Posted on April 4, 2019 by Aliya Eastham - Uncategorised

Pregnant women in England will be able to get a new type of blood test to check for the potentially life-threatening condition pre-eclampsia. (https://www.bbc.co.uk/news/health-47771688)
NHS England is making PLGF testing more widely available as evidence suggests it speeds up diagnosis which could save lives.
Mums-to-be who develop pre-eclampsia have dangerously high blood pressure which can damage vital organs.
The PLGF test tells doctors if a woman is at high, medium or low risk.
Pre-eclampsia affects tens of thousands of pregnancies each year, but can be managed if spotted early enough.
Those at higher risk should be very closely monitored and may have to have their baby delivered early if the condition becomes too severe despite treatment.
Sarah Findlay, 45 and from London, spent the last week of her pregnancy in hospital after medics discovered she had worryingly high blood pressure.
“It was a really stressful time. Up until that point my pregnancy had been amazing. Everything had been going really well,” she said.
“It was during a routine check-up that they noticed my blood pressure was far too high and they admitted me because they were concerned that it might be pre-eclampsia.
“I went from feeling like a mum to a patient. I was really terrified because I did not know if I would be OK and whether I might lose my baby.”
Doctors closely monitored Sarah’s condition and she went on to have a healthy baby girl, Isla, who is now four.

She welcomes any test that can help predict and reassure pregnant women about their risk of pre-eclampsia.
Trials of the new PLGF (placental growth factor) blood test, which costs about £70, show it speeds up diagnosis, meaning life-threatening complications to the mother and baby can be avoided.
More than 1,000 women at 11 UK maternity units took part in the trials during their second and third trimesters.
Using PLGF alongside regular blood pressure and urine checks cut the average time to diagnosis from four days to around two.
Earlier diagnosis was linked with a lower chance of serious complications – 5.3% (24 of 447 women diagnosed with usual checks) versus 3.8% (22 of 573 women diagnosed with usual checks plus PLGF).
Lead researcher Prof Lucy Chappell, from King’s College London, said: “This really is going to make a difference to women. The challenge for doctors is spotting which pregnancies are high risk and need closer monitoring. PLGF helps us reach that diagnosis earlier.”
Prof Tony Young, from NHS England, said: “The NHS, with partners in government, will be making this test more widely available across the NHS as part of our plans to ensure as many patients as possible can benefit from world-class health innovations.”
Posted on February 4, 2019 by Aliya Eastham - Uncategorised

The Pig is ready to give good vibes this year. This animal sign is a symbol of prosperity and good luck and horoscope experts say everyone will be blessed with good fortune and success in the Year of the Pig. The Pig has an authentic personality, hard worker, and energetic. Their enthusiastic personality enlightens everyone around them.
Posted on December 17, 2018 by Aliya Eastham - Uncategorised

The puerperium covers the 6-week period following birth, during which time the various physiological changes that occurred during pregnancy revert to the non-pregnant state Guzman 2010). Although for most women, the postnatal period is uncomplicated, care during this time needs to address any departures from expected recovery after birth.
Common puerperal problems include: pain in the perineal area, if the perineum has been damaged during the birth; urinary stress incontinence; painful or difficult urination; constipation; haemorrhoids; insufficient lactation, mastitis; breast abscesses; back pain; headache due to epidural/spinal anaesthesia; persistent fatigue; the ‘baby blues’; and postnatal depression (affects about 10%).
For pain in the perineum, cold compresses and analgesics may be used (NICE 2006). For urinary stress incontinence, the usual treatment is to teach and encourage pelvic floor exercises. For constipation and haemorrhoids, stool softeners may be needed. Making sure all milk is expressed is the first action with mastitis, and cold compresses may be used. If a bacterial infection is suspected, antibiotics are prescribed, while breast abscesses are treated with incision and drainage. Back pain and headache are managed in the same way as in the general population. Persistent fatigue can be the result of anaemia due to excessive blood loss, and may be treated with iron supplements or sometimes a blood transfusion. Women with the ‘baby blues’ need reassurance that it will pass quickly and is a ‘normal’ experience in the first week after giving birth (SIGN 2002). Those with postnatal depression are referred to psychological therapies and possibly given antidepressants (NICE 2007).
Guzman GM et al. Normal and abnormal puerperium. eMedicine 2010 [online]. Available:http://emedicine.medscape.com/article/260187-overview
National Institute for Health and Clinical Excellence, 2007. Antenatal and postnatal mental health: clinical management and service guidance. NICE Clinical Guideline, [online]. Available:
National Institute for Health and Clinical Excellence, 2006. Postnatal care: Routine postnatal care of women and their babies. NICE Clinical Guideline, [online]. Available: http://www.nice.org.uk/nicemedia/live/10988/30144/30144.pdf and http://www.nice.org.uk/nicemedia/live/10988/30146/30146.pdf
Scottish Intercollegiate Guidelines Network, 2002. Postnatal depression and puerperal psychosis, [online]. Available:
One systematic review of various treatments for breast engorgement during lactation (Manges 2010) located one eligible and analysable acupuncture study (Kvist 2007), and found that, compared to women receiving routine care, women receiving acupuncture had greater improvements in symptoms in the days immediately following treatment. The original study authors concluded that acupuncture plus care interventions such as correction of breast feeding position and babies’ attachment to the breast, might be more effective and less invasive than oxytocin nasal spray for inflammatory symptoms of the breast, however, the evidence is still very much at a preliminary stage.
In other randomised controlled trials, acupuncture and electro-acupuncture have been shown to delay the time to requesting pain relief medication after caesarean section, and to decrease the patient-controlled analgesia doses used within the first 24 hours (Wu 2009); both auricular acupressure using press seeds (Zhou 2009) and electroacupuncture (Wang 2007) have been found to have some efficacy in hypogalactia. [See Table below]
Also see other Factsheets, such as those for Acupuncture and Back Pain, Acupuncture and Migraines, Acupuncture and Anxiety, Acupuncture and Chronic Fatigue Syndrome, Acupuncture and Urinary Incontinence, Acupuncture and GI tract Disorders.
In general, acupuncture is believed to stimulate the nervous system and cause the release of neurochemical messenger molecules. The resulting biochemical changes influence the body’s homeostatic mechanisms, thus promoting physical and emotional well-being. Stimulation of certain acupuncture points has been shown to affect areas of the brain that are known to reduce sensitivity to pain and stress, as well as promoting relaxation (Hui 2010)
Acupuncture may increase milk production, help relieve pain (e.g. back pain, headache, pain in the perineum), and improve mood and reduce anxiety in women who have recently given birth by:
Posted on November 29, 2018 by Aliya Eastham - Uncategorised

The menopause, defined as the end of the last menstrual period, occurs at a median age of 53 years (Hardy 2005). The change in hormone levels during the perimenopause and menopause, particularly the decline in levels of oestrogen, can cause acute menopausal symptoms; for example, about 30-70% of women in Western countries will experience vasomotor symptoms, such as hot flushes and night sweats (Freeman 2007; Melby 2005). https://www.acupuncture.org.uk/a-to-z-of-conditions/a-to-z-of-conditions/menopausal-symptoms.html
Some women also report vaginal dryness and psychological symptoms, including tiredness, sleep disturbances, mood swings, forgetfulness and loss of libido (Melby 2005; Bachmann 1999). The median duration of menopausal vasomotor symptoms is about 4 years but, in around 10% of women, they last longer than 12 years (Polity 2008).
The most commonly used conventional medical treatment for such symptoms is hormone replacement therapy (HRT), comprising an oestrogen alone (in women who have had a hysterectomy) or in combination with a progestogen. HRT is now only indicated for short-term treatment of menopausal symptoms in the UK (MHRA 2007).
Bachmann GA (1999) Vasomotor flushes in menopausal women. Am J Obstet Gynecol 180: 312-6.
Freeman EW, Sherif K. Prevalence of hot flushes and night sweats around the world: a systematic review. Climacteric 2007; 10: 197-214.
Hardy R, Kuh D. Social and environmental conditions across the life course and age at menopause in a British birth cohort study. BJOG 2005; 112: 346-54.
Medicines and Healthcare products Regulatory Agency. Hormone-replacement therapy: updated advice. Drug Safety Update 2007; 1: 2-4.
Melby MK et al. Culture and symptom reporting at menopause. Hum Reprod Update 2005; 11: 495-512.
Politi MC et al. Revisiting the duration of vasomotor symptoms of menopause: a meta-analysis. J Gen Intern Med 2008; 23: 1507-13.
Systematic reviews (Lee 2009; Cho 2009) and randomised controlled trials published since these reviews were done (Kim 2010; Venzke 2010; Boroud 2010; Boroud 2009; Parks 2009; Avis 2008) have found: a) no difference between real and sham acupuncture for the treatment of menopausal symptoms, b) acupuncture is at least as effective, and sometimes superior to, hormonal drug treatment, c) additional acupuncture improves on usual, or self, care, and d) moxibustion is better than no intervention. These results suggest that sham acupuncture has therapeutic effects in itself, thus reducing its utility as a ” placebo” control for ‘true’ acupuncture. However, both reviews suggested that more high quality studies are needed to confirm this. (see Table overleaf)
Acupuncture may help reduce symptoms of the menopause and perimenopause by:
Acupuncture is a tried and tested system of traditional medicine, which has been used in China and other eastern cultures for thousands of years to restore, promote and maintain good health. Its benefits are now widely acknowledged all over the world, and in the past decade traditional acupuncture has begun to feature more prominently in mainstream healthcare in the UK. In conjunction with needling, the practitioner may use techniques such as moxibustion, cupping, massage or electro-acupuncture. They may also suggest dietary or lifestyle changes.
Traditional acupuncture takes a holistic approach to health and regards illness as a sign that the body is out of balance. The exact pattern and degree of imbalance is unique to each individual. The traditional acupuncturist’s skill lies in identifying the precise nature of the underlying disharmony and selecting the most effective treatment. The choice of acupuncture points will be specific to each patient’s needs. Traditional acupuncture can also be used as a preventive measure to strengthen the constitution and promote general wellbeing.
An increasing weight of evidence from Western scientific research (see overleaf) is demonstrating the effectiveness of acupuncture for treating a wide variety of conditions. From a biomedical viewpoint, acupuncture is believed to stimulate the nervous system, influencing the production of the body’s communication substances – hormones and neurotransmitters. The resulting biochemical changes activate the body’s self-regulating homeostatic systems, stimulating its natural healing abilities and promoting physical and emotional wellbeing.
With over 3000 members, the British Acupuncture Council (BAcC) is the UK’s largest professional body for traditional acupuncturists. Membership of the BAcC guarantees excellence in training, safe practice and professional conduct. To find a qualified traditional acupuncturist, contact the BAcC on 020 8735 0400 or visit www.acupuncture.org.uk
Research |
Conclusion |
Systematic reviews |
|
| Lee MS et al. Acupuncture for treating menopausal hot flushes: a systematic review. Climacteric. 2009; 12: 16-25.
|
A systematic review, including 6 randomised controlled trials, which assessed the effectiveness of acupuncture as a treatment option for menopausal hot flushes. Four trials compared the effects of acupuncture with sham acupuncture on non-acupuncture points. All of these trials failed to show specific effects on menopausal hot flush frequency, severity or index. One trial found no effect of acupuncture on hot flush frequency and severity compared with sham acupuncture on acupuncture points that are not relevant for the treatment of hot flushes. The remaining trial tested acupuncture against non-penetrating acupuncture on non-acupuncture points. Its results suggested favorable effects of acupuncture on menopausal hot flush severity. However, this study was too small to generate reliable findings. The reviewers concluded that sham-controlled randomised controlled trials have failed to show specific effects of acupuncture for the control of menopausal hot flushes. |
| Cho SH, Whang WW. Acupuncture for vasomotor menopausal symptoms: A systematic review. Menopause 2009; 16: 1065-73.
|
A systematic review, including 11 randomised controlled trials with a total of 764 patients, which assessed whether acupuncture therapy reduces vasomotor menopausal symptoms and evaluated the adverse effects of acupuncture therapy. Six trials compared acupuncture treatment to sham or placebo acupuncture. Only one study using a non-penetrating placebo needle found a significant difference in the severity outcomes of hot flashes between groups (mean difference, 0.48, 95% CI, 0.05 to 0.91). Five studies reported a reduced frequency of hot flushes within groups; however, none found a significant difference between groups. An analysis of the outcomes of the trials that compared acupuncture with hormone therapy or oryzanol for reducing vasomotor symptoms showed that acupuncture was superior. Three trials reported minimal acupuncture-related adverse events. The reviewers concluded that there was no evidence from trials that acupuncture is an effective treatment in comparison to sham acupuncture for reducing menopausal hot flushes, but that some studies have shown that acupuncture therapies are better than hormone therapy |
Review
|
|
| Borud E, White A. A review of acupuncture for menopausal problems. Maturitas 2010; 66: 131-4.
|
A review paper that looked at clinical trials of acupuncture for menopausal symptoms. The reviewers found that, for natural menopause, one large study has shown acupuncture to be superior to self-care alone in reducing the number of hot flushes and improving the quality of life; five small studies have been unable to demonstrate that the effect of acupuncture is limited to any particular points, as traditional theory would suggest; and one study showed acupuncture was superior to blunt needle for flash frequency but not intensity. For flushes associated with induced menopause, clearly acupuncture is useful for reducing flushes in clinical practice, but there is mixed evidence on the nature of the effect: one trial found genuine acupuncture superior to control needling, but another showed no significant difference between acupuncture and blunt needle. The possible mechanisms of acupuncture for hot flushes are discussed. |
Clinical studies |
|
| Kim KH et al. Effects of acupuncture on hot flashes in perimenopausal and postmenopausal women-a multicenter randomized clinical trial. Menopause 2010; 17: 269-80.
|
A randomised controlled trial that evaluated the effectiveness of acupuncture plus usual care for relief of hot flushes and menopause-related symptoms compared with usual care alone in perimenopausal or postmenopausal women.. The primary outcome was the mean change in the average 24-hour hot flash score (combining frequency and severity of flushes) at week 4 from baseline. The secondary outcome was the mean change in menopause-related symptoms as estimated by the Menopause Rating Scale questionnaire. Follow-up assessment at week 8 was conducted in the treatment group only. The mean change in the average 24-hour hot flush score was -16.57 in the treatment group and -6.93 in the control group (p<0.0001). The total Menopause Rating Scale score, as well as the subscale scores for the psychological, somatic, and urogenital dimensions of menopause, showed significant improvement in the acupuncture group compared with the control group (p<0.001). The researchers concluded that their results suggest that acupuncture in addition to usual care is associated with marked clinical improvement in hot flushes and menopause-related symptoms in perimenopausal or postmenopausal women. |
| Venzke L et al. A randomized trial of acupuncture for vasomotor symptoms in post-menopausal women. Complementary Therapies in Medicine 2010; 18: 59-66.
|
A randomised controlled trial that aimed to determine whether acupuncture would relieve the vasomotor symptoms of post-menopausal women. Fifty one women were randomly assigned to receive 12 weeks of treatment with either Traditional Chinese Medicine (TCM) acupuncture or shallow needle (sham) acupuncture. They all kept a diary recording their hot flashes each day. At baseline, study participants filled out Greene Climacteric Scales and the Beck Depression and Anxiety Inventories. These same outcomes were also measured at week 4 of treatment and at 1 week and 12 weeks after treatment. Both groups of women showed statistically significant improvement on all study parameters, but there was no difference between them. The researchers concluded that the results showed that both TCM and sham acupuncture were effective treatments of post-menopausal vasomotor symptoms, and that shallow needling may have therapeutic effects in itself, thus reducing its utility as a ” placebo” control for ‘true’ acupuncture |
| Borud EK et al. The Acupuncture on hot flushes among menopausal women (ACUFLASH) study, a randomized controlled trial. Menopause 2009; 16: 484-93.
Borud EK et al. The acupuncture on hot flashes among menopausal women study: Observational follow-up results at 6 and 12 months. Menopause 2010; 17: 262-8.
|
A randomised controlled trial that compared the effectiveness of individualized acupuncture plus self-care versus self-care alone on hot flushes and health-related quality of life in 267 postmenopausal women. Hot flush frequency (the primary endpoint) decreased by 5.8 per 24 hours in the acupuncture group and 3.7 per 24 hours in the control group (p<0.001). Hot flush intensity decreased by 3.2 units in the acupuncture group and 1.8 units in the control group (p<0.001). The acupuncture group experienced statistically significant improvements in the vasomotor, sleep, and somatic symptoms dimensions of the Women’s Health Questionnaire compared with the control group. Follow-up at 6 and 12 months found no significant difference between the groups. The researchers concluded that acupuncture can contribute to a more rapid reduction in hot flushes and increase in health-related quality of life in postmenopausal women,but probably has no long-term effects. |
| Park JE et al. Moxibustion for treating menopausal hot flashes: a randomized clinical trial. Menopause 2009; 16: 660-5.
|
A randomised controlled trial that evaluated the effect of moxibustion on hot flashes in 51 perimenopausal and postmenopausal women compared to a waiting list (control). The primary outcome measures were frequency and severity of hot flashes. By week 4, the difference in severity and frequency of hot flashes had become statistically significant between the treatment groups and the control participants. The researchers concluded that their results suggest that moxibustion reduces both the frequency and severity of menopausal hot flashes as compared with those in control participants. |
| Avis NE et al. A randomized, controlled pilot study of acupuncture treatment for menopausal hot flashes. Menopause 2008; 15: 1070-8.
|
A study that investigated the feasibility of conducting a randomised trial of the effect of acupuncture in decreasing hot flashes in peri- and postmenopausal women. Fifty-six women who had at least four hot flashes per day were given one of three treatment: usual care, sham acupuncture, or TCM acupuncture. Daily diaries were used to track frequency and severity of hot flashes. There was a significant decrease in mean frequency of hot flashes between weeks 1 and 8 across all groups (p=0.01), although the differences between the three study groups were not significant. However, the two acupuncture groups showed a significantly greater decrease than the usual care group (p<0.05), but did not differ from each other. Results followed a similar pattern for the hot flash index score. There were no significant effects for changes in hot flash interference, sleep, mood, health-related quality of life, or psychological well-being. The researchers concluded that their results suggest either that there is a strong placebo effect or that both traditional and sham acupuncture significantly reduce hot flash frequency |
| Xia XH et al. Multicentral randomized controlled clinical trials about treatment of perimenopausal syndrome with electroacupuncture of sanyinjiao (SP 6) [Article in Chinese] . Zhen Ci Yan Jiu. 2008 Aug;33(4):262-6.
|
A randomised controlled trial including 157 women with perimenopausal symptoms that compared electroacupuncture with nylestriol and medroxyprogesterone The therapeutic effect was evaluated by using a “symptoms-signs score scale”, and changes in serum estradiol (E2), follicle stimulating hormone (FSH) and luteotrophic hormone (LH). The Kupperman index was determined before and after the treatment and decreased significantly and similarly in both groups (p<0.01). Serum FSH and LH decreased and serum E2 increased significantly in the acupuncture group (p<0.01). Serum LH and E2 levels were significantly lower with acupuncture than with medication (p<0.05). The researchers concluded that electroacupuncture is able to regulate serum E2, FSH and LH levels and effectively improve perimenopausal syndrome. |
Research on mechanisms for acupuncture in general |
|
| Cheng KJ. Neuroanatomical basis of acupuncture treatment for some common illnesses. Acupunct Med 2009;27: 61-4.
|
A review that looked at acupuncture treatment for some common conditions. It is found that, in many cases, the acupuncture points traditionally used have a neuroanatomical significance from the viewpoint of biomedicine. From this, the reviewers hypothesize that plausible mechanisms of action include intramuscular stimulation for treating muscular pain and nerve stimulation for treating neuropathies.
|
| Lee B et al. Effects of acupuncture on chronic corticosterone-induced depression-like behavior and expression of neuropeptide Y in the rats.Neuroscience Letters 2009; 453: 151-6.
|
In animal studies, acupuncture has been found to significantly reduce anxiety-like behaviour, and increase brain levels of neuropeptide Y, the brain levels of which appear to correlate with reported anxiety.
|
| Samuels N et al. Acupuncture for psychiatric illness: a literature review. Behav Med 2008; 34: 55-64 | A literature review of acupuncture for psychiatric illness, which presents research that found acupuncture to increase central nervous system hormones, including ACTH, beta-endorphins, serotonin, and noradrenaline. It concludes that acupuncture can have positive effects on depression and anxiety. |
| Zhou Q et al. The effect of electro-acupuncture on the imbalance between monoamine neurotransmitters and GABA in the CNS of rats with chronic emotional stress-induced anxiety. Int J Clin Acupunct 2008 ;17: 79-84. | A study of the regulatory effect of electro-acupuncture on the imbalance between monoamine neurotransmitters and GABA in the central nervous system of rats with chronic emotional stress-induced anxiety. The levels of serotonin, noradrenaline and dopamine fell significantly, while GABA levels were significantly higher in the rats given acupuncture (P<0.05, or P<0.0). The researchers concluded that the anti-anxiety effect of electro-acupuncture may relate to its regulation of the imbalance of neurotransmitters.
|
| Zijlstra FJ et al. Anti-inflammatory actions of acupuncture. Mediators Inflamm 2003;12: 59-69. | A review that suggests a hypothesis for the anti-inflammatory action of acupuncture. Insertion of acupuncture needle initially stimulates production of beta-endorphins, calcitonin gene-related peptide (CGRP) and substance P, leading to further stimulation of cytokines and nitric oxide (NO). While high levels of CGRP have been shown to be pro-inflammatory, CGRP in low concentrations exerts potent anti-inflammatory actions. Therefore, a frequently applied ‘low-dose’ treatment of acupuncture could provoke a sustained release of CGRP with anti-inflammatory activity, without stimulation of pro-inflammatory cells.
|
| Pomeranz B. Scientific basis of acupuncture. In: Stux G, Pomeranz B, eds. Acupuncture Textbook and Atlas. Heidelberg: Springer-Verlag; 1987:1-18.
|
Needle activation of A delta and C afferent nerve fibres in muscle sends signals to the spinal cord, where dynorphin and enkephalins are released. Afferent pathways continue to the midbrain, triggering excitatory and inhibitory mediators in spinal cord. Ensuing release of serotonin and norepinephrine onto the spinal cord leads to pain transmission being inhibited both pre- and postsynaptically in the spinothalamic tract. Finally, these signals reach the hypothalamus and pituitary, triggering release of adrenocorticotropic hormones and beta-endorphin. |
Additional Info